There are three major types of cataract surgery, including phacoemulsification, extracapsular cataract extraction, and laser-assisted surgery.
Phacoemulsification is the most typical method, which uses ultrasound technology to break up the cataract for removal.
Extracapsular cataract extraction removes the clouded lens in one piece through a larger incision.
In laser-assisted surgery, sophisticated laser technology enhances the surgeon’s precision and efficiency.
Each type has unique advantages, based on the patient’s needs and the surgeon’s advice.Knowing the different types of cataract surgery available to you will allow you to make an informed decision.
What Is Cataract Surgery
Cataract surgery is a safe and effective procedure that restores clear vision by replacing the eye’s cloudy natural lens with an artificial intraocular lens (IOL). With a 90% success rate, it is one of the most common and trusted surgeries worldwide.
The procedure greatly improves quality of life by enhancing independence and mobility, reducing accident risks in older adults. Recovery is quick, with most people resuming gentle activities within a few days. Mild discomfort or blurred vision may occur initially but usually resolves fast. Advancements in surgical techniques continue to make cataract surgery safer and more effective.
Types of Cataract Surgery
Cataract surgery today offers several advanced options that were unimaginable just a generation ago. Each approach comes with unique procedures, recovery times, and benefits, allowing patients to choose the method best suited to their needs. Understanding these options is an important step toward making informed and empowered decisions about your eye care.
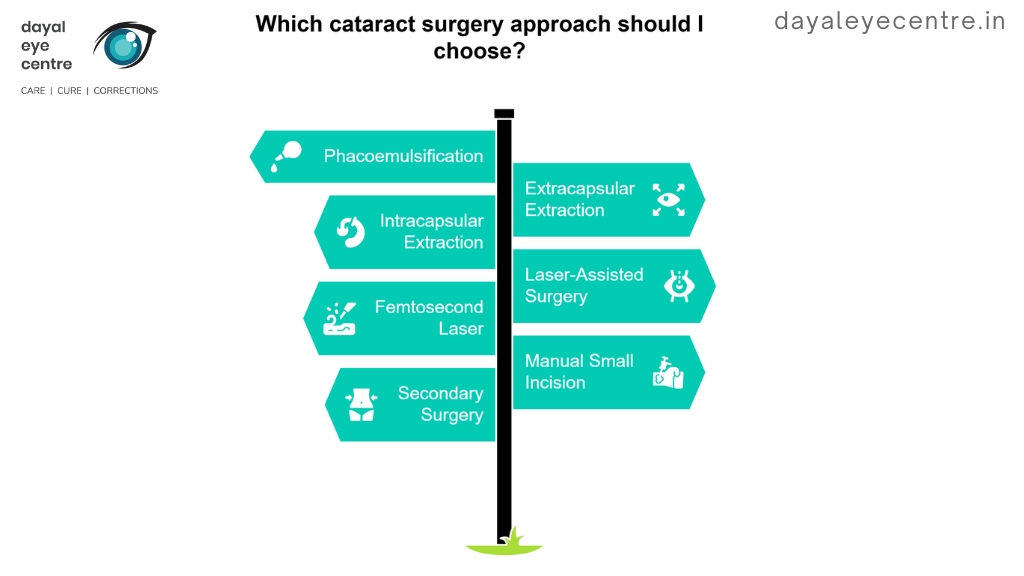
1. Phacoemulsification
- Most commonly performed today.
- Small incision (2–3 mm) in the cornea.
- Uses ultrasound to break up and remove the cloudy lens.
- An intraocular lens (IOL) is implanted for clear vision.
- Quick procedure (~30 minutes), minimal sedation, fast healing.
2. Extracapsular Cataract Extraction(ECCE)
- Used for advanced or dense cataracts unsuitable for phaco.
- Larger incision (10–12 mm), lens removed in one piece.
- IOL placed in the remaining posterior capsule.
- Requires sutures, longer recovery than phaco.
3. Intracapsular Cataract Extraction(ICCE)
- Rarely used today.
- Entire lens and capsule removed through a large incision.
- IOL placed in front of the iris.
- Reserved for extreme cases like severe trauma.
4. Laser-Assisted Cataract Surgery
- Uses lasers for corneal incisions and softening the cataract.
- Improves precision and uniformity.
- Faster recovery and improved visual results.
5. Femtosecond Laser-Assisted Surgery
- Advanced version of laser-assisted surgery.
- Femtosecond laser creates ultra-precise incisions and fragments the cataract.
- Faster recovery, better visual acuity.
6. Manual Small Incision Cataract Surgery(MSICS)
- Type of ECCE with smaller incision (~6–7 mm).
- Combines manual technique with smaller incision for quicker healing and less pain.
- Ideal when phacoemulsification is impractical (dense or complicated cataracts).
7. Secondary Cataract Surgery
- Treats posterior capsule opacification (PCO), a common post-surgery complication.
- Laser procedure clears clouding behind the IOL.
- Restores sharp vision quickly.
Benefits of Different Cataract Surgeries
Improved vision stability
- Vision becomes brighter, sharper, and glare is reduced.
- Over 90% of patients experience significant improvement.
- Advanced IOLs correct astigmatism and presbyopia.
Quick Recovery
- Most procedures are outpatient.
- Vision improvement within days; normal activity resumes in under a week.
- Minimal hospital stay or downtime.
Long-Term Vision Stability
- With proper IOL selection and post-op care, vision remains stable for years.
Enhanced Quality of Life
- Restores independence for daily tasks like reading, driving, and mobility.
- Reduces risk of accidents in older adults.
Cataract surgery today is not just about removing a cloudy lens—it’s about restoring functional vision, independence, and overall quality of life. Choosing the right surgical method depends on cataract type, severity, eye health, and lifestyle, making personalized consultation essential.
Risks and Complications of Cataract Surgery
Cataract surgery is the most common procedure performed in the world, with a greater than 95% success rate and less than 1% complication rate. Surgery is not without its risks, even for something as straightforward as cataract surgery. Although these risks are uncommon, knowing them will help you make educated decisions and be prepared for a quick recovery.
Possible risks include:
- Infection: Rare, but surgical-site infections can occur and require prompt treatment.
- Vision Loss: Although uncommon, complications during or after surgery can lead to partial or complete vision loss.
- Inflammation: Some patients may experience post-surgical inflammation, typically managed with prescribed eye drops.
- Retinal Detachment: Particularly in high-risk patients (e.g., severe myopia), retinal detachment is a rare but serious complication
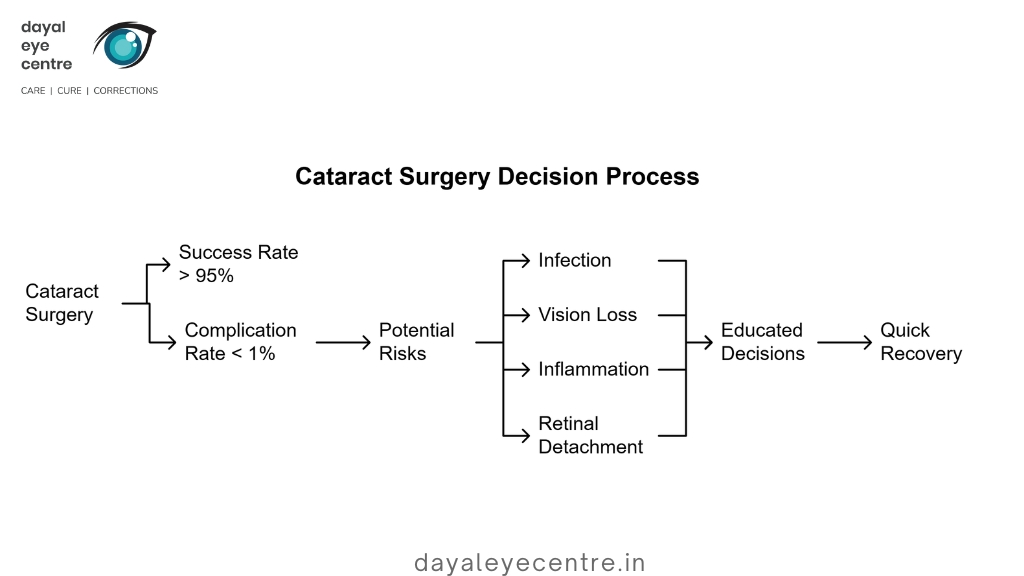
With skilled surgeons and proper post-operative care, these risks are minimized, making cataract surgery a safe and effective option for restoring vision.
Cataract Surgery Risks and How to Choose the Right Procedure
Cataract surgery is generally very safe, but understanding potential risks and how to select the best surgical option is important for optimal outcomes.
Risk of Infection
Maintaining a sterile environment during surgery is critical to prevent infections. The risk is minimized through pre- and post-operative antibiotic eye drops.
Warning signs: redness, swelling, or discharge from the eye.
Thanks to strict surgical protocols, infections occur in less than 1% of patients.
Potential Vision Loss
Vision loss is exceptionally rare, occurring in less than 1 in 1,000 patients. Serious complications such as retinal damage or severe intraocular inflammation may be responsible.
Patients with underlying eye conditions may have a slightly higher risk, so a thorough pre-operative evaluation and selection of an experienced surgeon is crucial
Post-Surgery Inflammation
Mild inflammation is relatively common and typically resolves within a few days. Prescription anti-inflammatory eye drops help manage this effectively.
The majority of patients experience no permanent complications.
Risk of Retinal Detachment
Although extremely uncommon, retinal detachment can occur after cataract surgery.
Warning signs: new floaters or flashes of light—urgent evaluation is required.
High-risk patients should be monitored more closely post-surgery, but modern techniques keep this risk minimal.
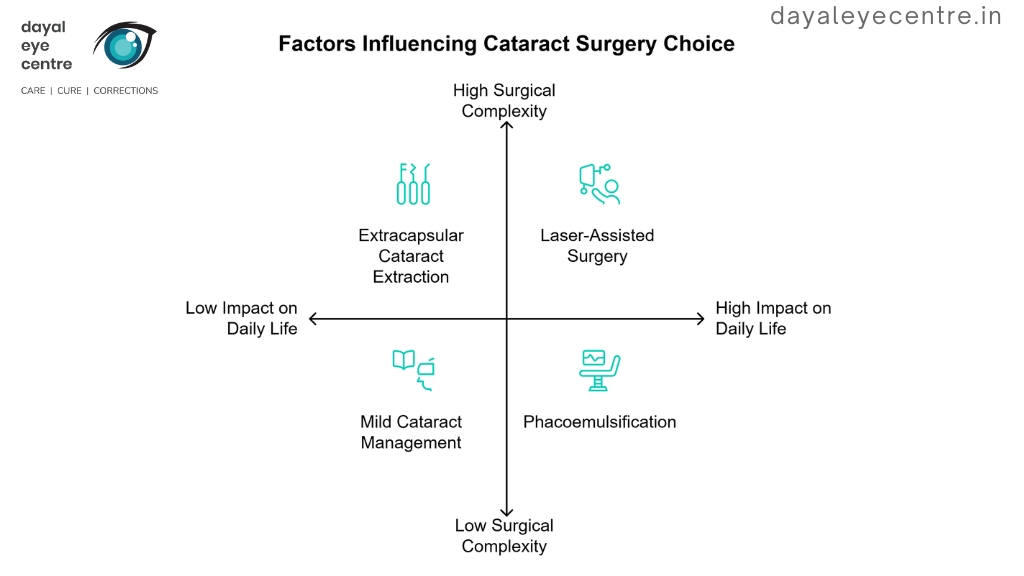
Choosing the Right Cataract Surgery
Selecting the right procedure is a personalized decision based on the severity of your cataract, your vision needs, and overall eye health.
Key Considerations include:
- Impact on daily life: Difficulty driving at night, reading, or dealing with light sensitivity should be discussed with your ophthalmologist.
- Symptom tracking: Monitoring changes in vision clarity, glare sensitivity, or focusing ability helps your doctor choose the best approach.
- Health history: Prior eye surgeries, existing eye conditions, or systemic health issues may influence which surgical method is safest and most effective.
- Risks vs. benefits: A clear understanding of potential complications helps patients make informed decisions.
- Logistics and lifestyle: Recovery time, work schedule, and support at home can influence the timing and type of surgery.
By communicating openly with your eye specialist, you can ensure a tailored surgical plan that maximizes your chances of excellent visual outcomes.
Preparing for Cataract Surgery
Before surgery, it’s important to plan for logistics and recovery:
- Bring a companion: You will likely need a friend or family member to accompany you and help with transportation afterward.
- Follow pre-op instructions: Simple steps such as eyelash cleaning with baby shampoo or fasting after midnight are common requirements.
- Post-surgery recovery: Most patients experience a full recovery by 8 weeks, but following your physician’s instructions closely will support a smooth and successful outcome.
Conclusion
Cataract surgery is a safe, effective, and life-changing procedure that restores clear vision and improves quality of life. Each surgical type has its advantages, and selecting the right approach depends on your vision needs, lifestyle, and overall health.
Open communication with your ophthalmologist ensures you can make well-informed decisions about your care. Remember, cataract surgery isn’t just about removing the clouded lens—it’s about regaining vision in a way that fits your life. Taking steps today to prioritize your eye health, including proper nutrition and regular check-ups, will keep your world bright and clear.
Frequently Asked Questions
-
What is cataract surgery?
Cataract surgery is the procedure used to remove the cloudy lens from your eye. The surgeon will then remove it and replace it with a clear, artificial lens. It gives people back vision that was dulled by cataracts.
-
What are the main types of cataract surgery?
The two most common types include Phacoemulsification (Phaco) and Extracapsular Cataract Extraction (ECCE). Phaco, which uses ultrasound, and ECCE, which requires a larger incision to extract the lens.
-
What is laser cataract surgery?
In laser-assisted cataract surgery, your surgeon utilizes advanced lasers to make precise incisions and fragment the lens. It provides greater precision and could result in less recovery time than more invasive techniques.
-
Are there benefits to choosing laser-assisted surgery?
Indeed, with laser-assisted surgery, there is increased accuracy, decreased risk and faster recovery. It’s regularly advised for individuals with difficult cataracts or astigmatism.
-
What are the risks of cataract surgery?
Rare risks of cataract surgery include infection, inflammation, or vision problems such as glare. These are extremely unusual and curable. Your surgeon will do everything possible to reduce risks through appropriate care.
-
How do I choose the right cataract surgery?
Talk through your goals and lifestyle with your ophthalmologist. Considerations such as overall eye health, lifestyle, and budget will help you determine which choice is best for you.
-
Is cataract surgery safe?
Yes, cataract surgery is one of the safest and most successful surgeries. The majority of patients enjoy better vision and few complications.






